What is an insulin Pump ?
An insulin pump is a battery operated portable device about the size of a pager, worn externally to deliver a continuous amount of fast-acting insulin. The wearer can also administer extra (bolus) doses of insulin when needed by pushing a button on the pump. Insulin pump treatment is a type of intensive insulin therapy requiring multiple insulin injections.
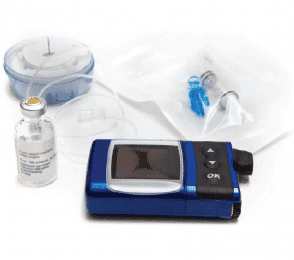

Insulin pumps have been in use for more than 20 years.
How an insulin pump works
An insulin pump delivers a continuous and automatic (basal) dose of insulin via a cannula (a small tube) inserted under the skin. A thin tube connects the cannula to the pump’s insulin reservoir (or cartridge). The cannula and tube should be changed every two to three days. The cannula is inserted under the skin using a tiny needle that is then removed.
An insulin pump attempts to mimic the function of a normal pancreas by delivering a basal insulin dose, and bolus doses at mealtime when blood glucose (sugar) levels rise above normal. Unlike the pancreas, insulin pumps don’t automatically deliver the appropriate amount of insulin based on what the user has eaten. Users, with the help of their healthcare team, must program the doses themselves. Consequently, they must monitor their glycemia closely, and precisely calculate the amount of carbohydrates ingested in order to adjust the insulin doses to be delivered.
Risks and Advantages
Benefits
Better glycemic control
Studies of diabetic children and adults indicate that insulin pump therapy generally provides better blood glucose (sugar) control, by reducing glycemic spikes and troughs, than treatment by multiple injections.
Greater freedom
One of the main benefits of an insulin pump is lifestyle – more freedom. Children and teens especially benefit, as they often have unpredictable schedules. A user can spontaneously decide when and how much insulin to administer.

A helpline lets the user take quick action if the pump breaks or if there is a technical problem.
Risks
Mechanical problems
Insulin pumps deliver fast-acting insulin whose effect lasts only three to four hours. Any unplanned interruption in insulin delivery can cause hyperglycemia, or even diabetic acidosis, if several hours elapse before the user corrects the problem. This can happen if a tube gets kinked or blocked, if the pump becomes dislodged, or even if the user forgets to change the empty insulin cartridge or replace a dead battery.
However, these risks can be eliminated thanks to preprogrammed alarms on the pump and by frequently checking your blood glucose (sugar) levels to detect any abnormal variations.
Risk of infection
Infection can arise if the cannula stays under the skin too long. On the other hand, if you change the cannula according to the recommended frequency (normally every two to three days), use the right technique and cleanse the skin properly, this risk can be avoided.
A treatment for everyone ?
An insulin pump can be an excellent way to manage your diabetes, but it won’t make it disappear. Insulin pump therapy requires significant involvement by the person with diabetes. For safety and effectiveness, it requires extra vigilance.

Insulin pump therapy requires significant involvement by the person with diabetes.
You could be an ideal candidate for an insulin pump if you:
- have a good understanding of your diabetes
- understand the impact of diet, physical activity, stress and insulin on your glycemic control
- are willing to measure your blood glucose (sugar) levels at least four times per day (often more often) and keep a record of the results
- are willing and able to learn how to count carbohydrates very precisely (using the advanced method)
- are monitored by a healthcare professional (physician or diabetes educator) who knows how insulin pumps work and can be contacted easily
- are willing to wear the device at all times and do regular maintenance (change the infusion kit, etc.)
When treatment begins, you need to be closely monitored by your healthcare team, to determine the basal insulin dose to be delivered and the required bolus doses. You will need to take training to learn how to use insulin pump therapy to properly manage your diabetes.
If this type of treatment interests you, talk to your healthcare team, who can help you make an informed decision.
Costs
An insulin pump costs about $7,000, plus another $1,500 to $3,000 per year for supplies (insulin cartridges, infusion kit (cannulas and tubes), adhesive patches, batteries, etc.).
Since 2011, the Régie de l’assurance maladie du Québec (RAMQ) has been reimbursing the cost of insulin pumps for Quebec children under the age of 18 who meet certain clinical criteria. Access to this program continues after 18 years of age for those who were signed up for the program at a younger age since its inception in 2011. Click here for more information about the RAMQ’s Insulin Pump Access Program.
Some group insurance plans cover some of the cost of an insulin pump and its supplies upon receipt of a physician’s letter attesting to the medical necessity of the device.
