Get a better understanding of insulin and other injectable medications.
Best Practices in Injection Technique
The following recommendations apply to people with diabetes being treated with insulin injections or GLP-1 analogues (albiglutide (EperzanTM), dulaglutide (Trulicity®), exenatide (Byetta®), exenatide sustained release (Bydureon®) and liraglutide (Victoza®)). They are based on the Recommendations for Best Practice in Injection Technique (2015) from the Forum for Injection Technique (FIT).

A healthcare professional trained in injection techniques can teach you how to do it right
Preparing for injection
Follow these important steps before an injection:
- Wash your hands and the injection site with soap and water, and dry well.
- If you use an alcohol swab (e.g.: in a hospital), let the skin dry completely before administering the injection.
- Check that the vial or cartridge has not passed its expiration date.
- Wipe the cartridge or vial with an alcohol swab.
When using cloudy insulin, gently roll the cartridge, vial or pen device 10 times, then tip it (do not shake) 10 times. Finally, inspect it to ensure that the suspension has a consistently milky white appearance.
Is a skin lift necessary?
In adults, a skin lift is used in some situations, based on needle length and the amount of adipose (fat) tissue. A skin lift should be used when the needle is 8 mm or longer. In addition, in people whose arms and legs or abdomen have little fatty tissue, a skin fold might be justified when using a needle of 5 mm or 6 mm. A skinfold may not be necessary especially when using a 4 mm needle .
A skin lift, if required, must be done properly to ensure that the medication is not injected into the muscle or not deeply enough.
Injection areas
In adults, the recommended injection areas are the following:
- abdomen
- thighs
- upper buttocks
- back of the upper arm (not a preferred area because of the difficulty reaching it when self-injecting)
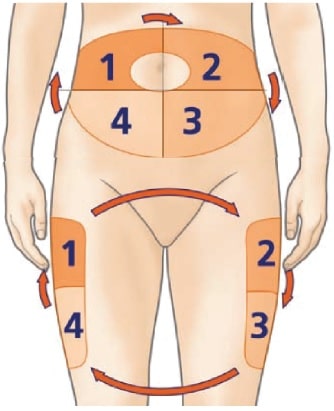
Insulin absorption can vary due to several factors, including the insulin injection sites. Insulin is absorbed more quickly when injected into the abdomen, compared to average absorption in the arms and thighs. The buttocks absorb insulin more slowly. GLP-1 analogues, on the other hand, appear to be absorbed at the same rate in the usual injection sites (abdomen, arms, and thighs).
Injecting insulin into an area used during physical activity may increase insulin absorption, resulting in faster action and a decrease in blood glucose (sugar) levels.
The rotation of injection areas and sites
To avoid the formation of skin dents and lumps (lipodystrophy) and to ensure consistent insulin absorption:
- Use a new needle for every injection.
- Regularly examine and palpate your injection areas for any signs of lipodystrophy.
- Vary the injection area and use a structured rotation within the same injection area.
Rotating anatomical areas
Insulin absorption varies from one anatomical region to another. Therefore, varying the regions is recommended, while reserving the same anatomical region for a particular time of day. For example, you can use the abdomen at breakfast and lunch, then the thighs at supper and bedtime.
Rotation des points d’injection
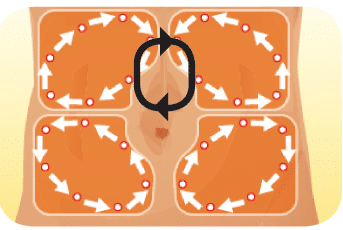
A structured rotation is recommended within the same anatomical region, leaving at least 1 to 2 cm (1 finger width) between each site and not using the same site for a month. For the abdomen, care should be taken to avoid injecting within 2 to 3 cm from the umbilicus (belly button).
To help you do this, divide each anatomical area into quadrants (four zones) and rotate the injection sites within the same quadrant for a week. Do likewise for the other three quadrants.
Avoiding pain
Some tips for making injections more comfortable:
- Use short needles (4 mm, 5 mm or 6 mm) to avoid intramuscular injections.
- Use a new needle for every injection.
- Keep injectable medication currently in use at room temperature.
- Avoid injecting into hair roots, scars, beauty marks or any other skin abnormality.
- If you use alcohol swabs, inject only after the alcohol has completely evaporated and the skin is dry.
- Insert the needle through the skin using a quick, smooth movement, then inject the medication slowly and evenly.
If, despite these tips, injections are still painful, consult a healthcare professional, who can check your technique and, if required, suggest other measures.
Storing insulin
Once a vial or cartridge has been opened, it should not be used for more than 28 days (42 days for insulin detemir). Unopened vial or cartridge of insulin should be stored in the refrigerator (2 to 8oC). Insulin should never be frozen or exposed to extreme heat (above 30 C) as this will affect its potency and alter its action.
After injecting, safely dispose of the needle and all sharps in an approved biomedical disposal container.
